Problems After Radiation Treatment for Prostate Cancer
Radiation therapy is an essential treatment for prostate cancers. Complications from radiation are very rare, but occasionally men can develop a urethral stricture after radiation treatment. The radiation, even many years after treatment, can cause the urethra or urinary channel to scar. When the urethra scars, men have difficulty in passing their urine and have obstruction of their flow. This leads to symptoms like urinary urgency and frequency, incontinence due to overactive bladder, or overflow of a full bladder, pain, and bladder infections.
Often this damage occurs in the first few years after treatment, but can also happen many years later, even after the prostate cancer has been completely cured. These strictures can be very hard to treat because the radiation damages the surrounding tissues and the urethra has a hard time healing after surgery.
This is a modal window.
Treatments
Basic treatments procedures for this complication include:
- Internal dilation/scope procedure - After radiation, internal dilations or scope procedures to cut the scar rarely will cure a stricture of the urethra.
- Catherization - Some patients have a permanent catheter placed through the abdomen into the bladder called a suprapubic tube, and others will perform self-catheterization of the urethra once a day to keep the stricture open. However, many patients do not like having a permanent catheter and find self-catheterization very painful.
- Surgery - In patients for whom a catheter doesn't work, a surgery can be done to remove the scar tissue and reconnect the urethra to the prostate. We have had many successes with this surgery at University of Utah Health despite the radiation damage to the urethra.
Surgery to Reconnect the Urethra
Different surgeries are done for different circumstances. For instance in some men the entire urethra through the prostate is scarred from radiation or attempts to clear the channel with scope procedures. In this circumstance the prostate needs to be removed and the urethra can be connected to the bladder (salvage prostatectomy).
In other patients, when the scarring is limited to the bottom of the prostate, a surgery through the perineum (the space between the scrotum and the anus) can be performed to remove the scar tissue and reconnect the urethra to the prostate (urethroplasty).
Figures: Two examples of radiation damage from prostate cancer treatment causing a stricture or scar at the junction of the lower prostate and the urethra. 1) The first is from implanted brachy therapy seeds. 2) The second is from the combination of high dose brachytherapy and external beam radiotherapy.
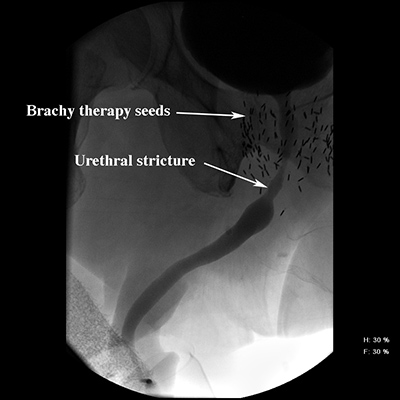
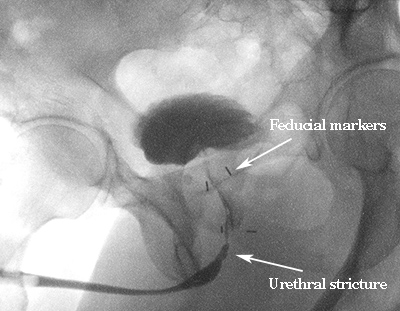
Urinary Control After Surgery
Most often scarring after radiation involves the urinary sphincter muscle at the bottom of the prostate (external sphincter). The sphincter muscle allows men to keep urine in their bladder and prevents leakage. Fortunately, men have two sphincter muscles and there is one at the opening of the bladder where the bladder meets the prostate (internal sphincter). Even if the lower sphincter is destroyed because of the radiation damage, the upper sphincter can keep men from leaking urine.
In some circumstances, however, the upper sphincter does not work or needs to be removed because the scarring is extensive. If this happens then patients need to have an artificial urinary sphincter placed after they have healed from the urethral surgery.
Artificial Urinary Sphincter (AUS)
An artificial urinary sphincter (AUS) is a silicone donut, which is placed around the urethra (the cuff). This sphincter or cuff is connected internally to a pump within the scrotum and a reservoir in the abdomen. The pump sits next to the testicle and when someone wants to urinate they squeeze the pump and the cuff deflates and allows urine to flow. Over the next two minutes or so the cuff self inflates and puts pressure back on the urethra.
Wait Time for Artificial Sphincter Placement
Unfortunately patients need to wait long enough to make sure that the urethra has completely healed. This is about three months after the catheters are all removed from the urethral surgery. Then another surgery is done to place the artificial sphincter around the urethra.
Improving Surgical Outcome
Your surgeon may talk to you about the use of hyperbaric oxygen. Hyperbaric oxygen involves going to a wound care center and having 20–40 treatments in a dive chamber with very highly concentrated oxygen. These treatments last about one to two hours and are usually done once a day. Hyperbaric oxygen treatment may improve the damage surrounding the scar tissue and may make the surgery more successful.
Unfortunately the hyperbaric oxygen treatment will not cure the stricture. Not every place has hyperbaric oxygen treatment center, and in patients where this is not available, the surgery can still be successful. Another thing your surgeon might recommend is laying a piece of muscle from your inner thigh underneath the area of surgery. This may act to increase the blood supply to the area of the surgery and protect the area from complications of very slow healing.
Will this surgery really work?
The outcomes of this type of surgery is not as good as urethral stricture surgery that is done without radiation damage, but we have gotten this surgery to work out well in many patients. Many patients have come to see us believing that nothing can be done because of the information they have been told about radiation damage. Usually we can find some plan that will improve patient’s quality of life even if the damage from radiation is severe.
