The Moran Eye Center is among a select group of institutions evaluating a unique simulator-based training system developed to help turn the tide of cataract blindness worldwide.
As the leading U.S. academic institution supporting local and international outreach work with dedicated resources, the John A. Moran Eye Center offers residents and fellows a range of extraordinary opportunities.
From exchange programs to release time for volunteer outreach work, Moran trainees can access a network of global partnerships working to reduce the burden of blindness worldwide. Part of the Moran experience includes in-depth training in Manual Small-Incision Cataract Surgery (MSICS), a technique used successfully in low-resource and remote parts of the world.
In the spring of 2021, Moran faculty and students will begin training on and evaluating the cutting-edge eye surgery simulator and courseware developed by HelpMeSee, an international nonprofit organization. HelpMeSee selected Moran—one of the few U.S. academic programs offering MSICS training as part of its curriculum—as an evaluator for the virtual reality, immersive simulation-based, instructor-led training system.
Moran Vice Chair of Education Jeff Pettey, MD, MBA, said the simulator could be a game-changer in quickly training more surgeons in the U.S. and low-resource nations in the MSICS technique.
Pettey recently co-authored a study published in Scientific Reports that concluded surgeons who trained on the HelpMeSee Simulation-Based Training System performed better in "real life" surgery compared to conventionally trained groups. Researchers observed a reduction in surgical errors of almost 50% as the HelpMeSee trainees began operating on live patients.
In the past ten years, Moran’s Global Outreach Division has worked in more than 25 countries as part of its mission to create sustainable eye care systems. Physicians and volunteers conduct high-volume surgery clinics to alleviate a backlog of blindness and train local doctors and nurses who can then teach others to increase access to care.
"I have admired Moran Eye Center for many years," said James Ueltschi, co-founder and chairman of HelpMeSee. "Jeff Pettey’s record there speaks for itself. Moran and Jeff’s embrace of MSICS as a critical skill for surgical ophthalmologists and its potential to end cataract blindness with widespread adoption throughout the developing world makes Moran a natural fit.
"Our MSICS training system, which was adapted from many decades of experience in commercial pilot training, brings, for the first time, a very high-fidelity surgical simulation experience along with objective measurements of the training results," Ueltschi continued. "With the help and support of Moran Eye Center, we are excited about the future, where access to cataract treatment is the rule rather than the exception wherever you live."
A Dire Need

Global blindness from cataracts has reached epic proportions—to the tune of 100 million visually impaired people. Of those, 17 million are bilaterally blind, and 83 million have moderate to severe vision loss.
For each visually impaired person, 2.5 people are taken out of the workforce or denied an education to care for them. Blindness is also associated with higher poverty rates, loss of social standing, isolation, depression, injuries, and earlier mortality.
According to the International Agency for the Prevention of Blindness (IAPB), without immediate action, the problem will double by 2050. But there are simply not enough surgeons trained to perform cataract surgeries in the world's poorest regions with the highest vision loss rates: Africa, China, South and Southeast Asia, and Latin America.
"Cataract surgery in the U.S. and other high-income countries is performed using phacoemulsification machines that aren't always practical for low-resource settings," explained Pettey. "MSICS is an elegant form of manual surgery where we remove the cloudy lens of a cataract—including complex, dense cataracts—without ultrasound technology. Most of all, it's safe and cost-effective."
Enhancing the Curriculum
Although MSICS has long been a part of the Moran curriculum, residents may not have an adequate exposure to the technique to be fully proficient by graduation. The eye surgery simulator will enhance and increase competence in the technique while serving as a source of valuable feedback to the HelpMeSee team.
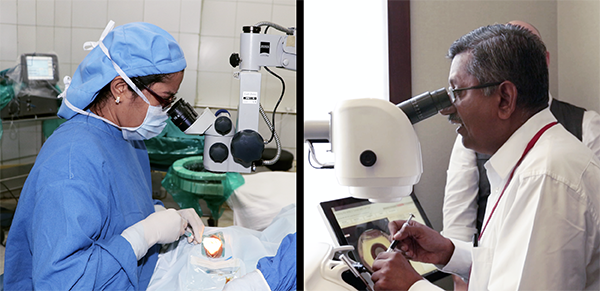
HelpMeSee is building a large-scale sustainable training model. It has already deployed the simulation-based training system with well-known institutions in several areas with the highest vision loss rates. Locations include India-based Aravind Eye Care System and L V Prasad Eye Institute; Zhongshan Ophthalmic Center, He Eye Specialist Hospital, and Eye Hospital, Wenzhou Medical University, in China; and the Mexico Institute of Ophthalmology.
There are four of the eye surgery simulators in the United States and Europe: the Moran Eye Center, Bascom Palmer Eye Institute at the University of Miami, Columbia University, and the Copenhagen Academy for Medical Education and Simulation.
"Adoption of MSICS could effectively accelerate high-volume treatment and begin to reduce the cataract surgery backlog," said HelpMeSee President and CEO Saro Jahani. "We cannot do it alone, of course. That's why we have established strategic partnerships to build the momentum and a sense of urgency to move swiftly to a competency-based simulation training model that provides eye surgeons with the ability to build proficiency without risk to patients to what they are most passionate about—restoring sight and restoring lives."
Innovation, Technology, and Training
With a shorter learning curve than that for phacoemulsification, MSICS simulation-based training offers a way to transfer surgical skills rapidly and effectively.
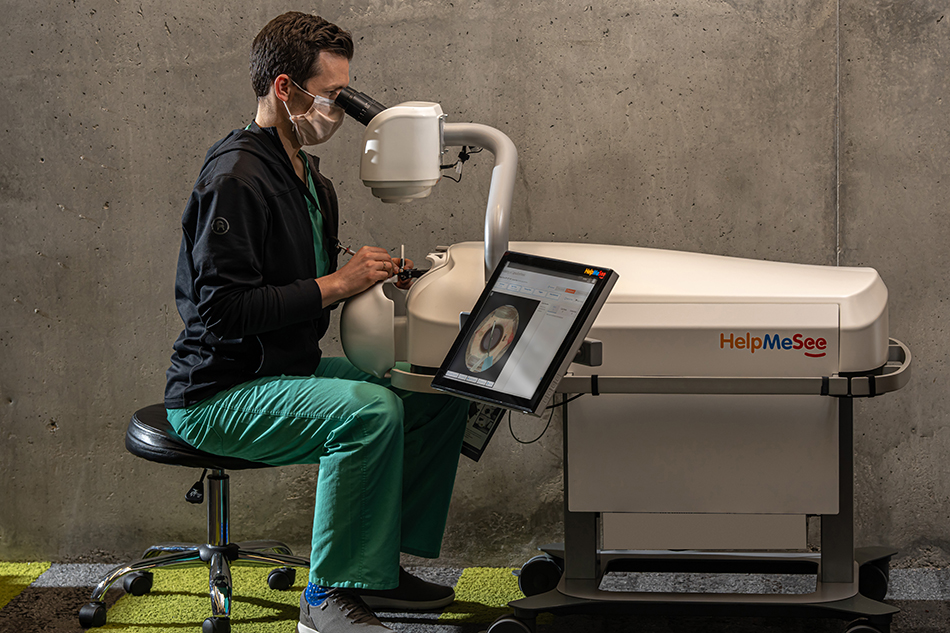
"The eye surgery simulator itself is a superb piece of technology," said Pettey. "As you look through a virtual reality image and place instruments on the eye in your view, you can actually feel the feedback from the simulated structures. It feels identical to the tissues of a human eye.
"We're still learning about the eye surgery simulator here at Moran," Pettey continued. "We don't yet know how long it will take a resident to gain full competency using the HelpMeSee Simulation-Based Training System. But it could potentially fast-forward residents to a level of a surgeon who's done 50 cases by the time they have their actual first real case."
How it Works
The HelpMeSee Simulation-Based Training System utilizes metrics to objectively measure competency to shorten the time it takes for surgeons to build proficiency and confidence before beginning live surgical training.
- Training methods include:
- Self-study (Ebook)
- Instructor-led "reverse classroom" sessions
- Hands-on lab exercises
- Simulation-based training
- Feedback sessions with HelpMeSee
Highlights:
- The simulator delivers lifelike physical representations, with a patient's body and head on a surgical table.
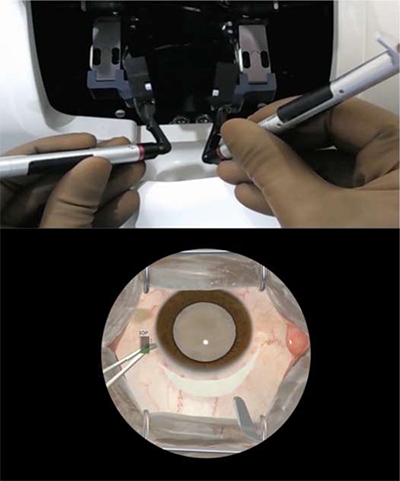
- Trainees use two handpieces that act as virtual instruments, which interact realistically with the eye model.
- The simulator provides true-to-life tactile feedback. As the trainee progresses, the simulator measures and reports performance data. Soft tissue physics modeling combined with haptic feedback give the trainee an accurate feel of how instruments interact with various tissue layers in the eye. This helps build muscle memory as the trainee operates. The HelpMeSee high-fidelity eye surgery simulator is the only one offering tactile, or haptic, feedback.
- Realistic visuals display eyeball simulation in stereoscopic 3D renderings. The trainee can instantly see any error or complication on the screen. They can see if a cut is standard, too deep, or too shallow—including bleeding or hitting another tissue layer if the cut is too deep.
- Trainees have access to unlimited practice sessions to repeat the individual steps of the MSICS procedure until they're proficient.
The Global Challenge of Cataracts
- Cataracts are the leading cause of blindness and a significant cause of visual impairment across the globe.
- One hundred million people worldwide need cataract surgery.
- Over 17 million people are bilaterally blind from cataracts in the world in 2020— 40% of all cases of blindness.
- The proportion of blindness due to cataracts among all eye diseases ranges from 15% in high-income regions to 50% or more in poor and remote areas.
- Because prevalence increases with age and is higher in females than males, cataract surgery remains an important focus for alleviating vision loss and addressing gender equity.
SOURCE: The International Agency for the Prevention of Blindness (IAPB)