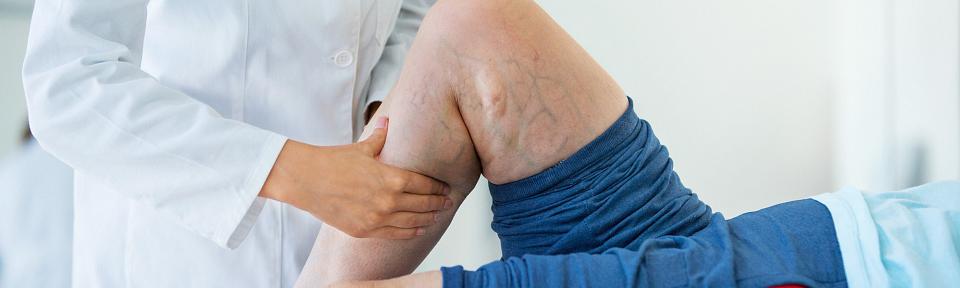
What Is Venous Insufficiency?
Venous insufficiency is a condition that affects the way blood flows in your body. When your veins are working normally, they return blood from all your organs to your heart. Tiny valves inside these veins keep the blood flowing in the right direction.
Venous insufficiency occurs when these valves aren’t working correctly. Blood may leak backward, away from the heart, causing blood to pool in your legs. This condition may affect the deep veins (these help propel blood towards your heart) or superficial veins (located closest to the skin's surface) of your legs. Some people with venous insufficiency also have deep vein thrombosis (DVT). DVT occurs when a blood clot forms in a vein located deep inside your body.
Why Choose U of U Health for Treatment?
Fellowship-trained, board certified vascular surgeons at University of Utah Health provide expert care for people with venous insufficiency. They will create a personalized treatment plan that may include non-surgical and surgical strategies, including minimally invasive endovenous laser therapy.
Risk Factors for Venous Insufficiency
Venous insufficiency is more common in people over the age of 50 and affects more women than men.
Sometimes, chronic venous insufficiency happens for unknown reasons. But you may be at higher risk for venous insufficiency if you have:
- experienced significant weight loss or weight gain (for example, women who have had multiple pregnancies are at higher risk for venous insufficiency since they have gained and lost weight several times);
- a family history of venous insufficiency or varicose veins;
- lifestyle concerns, such as being overweight, being sedentary, and smoking; or
- previous damage to one of your legs due to an injury, surgery, or blood clots, including deep vein thrombosis (DVT).
Venous insufficiency is less likely in people who are physically active since exercise and good muscle development in the calves can encourage the flow of blood.
Find a Venous Insufficiency Provider
Treatment Locations
We offer venous insufficiency treatments at the following locations:
Signs & Symptoms of Venous Insufficiency
The most common symptom of venous insufficiency is the onset of swelling in the legs and ankles after standing for periods of time. Other symptoms may include:
- pain, tiredness, tightness, or a burning feeling in your legs, which often worsen as the day goes on;
- discomfort and heaviness while walking that goes away when you rest or elevate your legs;
- patches of brown-colored or “leathery” skin, usually near your ankles;
- flaky and itchy skin on your legs or feet; and
- varicose veins (although many people with varicose veins do not have venous insufficiency).
Treatment is most effective when it begins in the early stages of venous insufficiency. If you are experiencing any of these signs or symptoms, make an appointment with your primary care provider or a vascular surgeon.
This condition does not go away on its own. Without treatment, venous insufficiency can lead to serious complications. For example, if the swelling in your ankles and legs becomes severe, you can develop ulcers and chronic wounds.
Diagnosing Venous Insufficiency
Vascular surgeons at U of U Health offer a thorough evaluation, diagnosis, and personalized treatment plan for people with symptoms of venous insufficiency. During the evaluation, the vascular surgeon will perform a complete medical history and physical, including an examination of your legs. You also will have a test called a venous reflux study.
What Is a Venous Reflux Study?
This test uses ultrasound imaging to show how blood is flowing through your veins in real time. It helps the vascular surgeon see the blood flow in your vein and determine whether the blood is leaking in the wrong direction.
During this test, you will lie down on an exam table. An ultrasound technologist will place a transducer (small, handheld device) on the skin where the affected vein is located. The transducer sends sound waves to the vein, and the ultrasound machine creates an image of the vein on a monitor.
At the end of the first appointment, the vascular surgeon will talk to you about your test results and treatment recommendations.
Non-Surgical Treatment Options
The first line of treatment for chronic venous insufficiency is to try non-surgical strategies. The goal is to promote normal flow of blood through the veins and reduce the pooling of blood in your legs. These conservative strategies may include:
- wearing compression stockings
- avoiding standing or sitting for long periods,
- exercising regularly (walking is a good choice),
- losing weight if you are overweight,
- elevating your legs frequently so that they are above the level of your heart,
Compression Stockings
Compression stockings apply pressure to your lower legs to improve blood flow. They can reduce symptoms of venous insufficiency, such as pain and swelling.
If you have had venous insufficiency for a while, you may already have tried using compression stockings. Your vascular surgeon may talk to you about using medical grade stockings to see if those are more effective.
These come in a variety of compressions and styles and may provide greater compression than stockings you have used previously.
Other Treatment Options for Venous Insufficiency
If non-surgical strategies are not successful, the vascular surgeon may recommend other options, such as:
- minimally invasive endovenous therapy or
- open surgery.
The goal of these procedures and surgeries is to remove or neutralize diseased veins closest to the surface of your skin. Afterward, “deep veins” in your leg will take over the job of returning blood to your heart.
Minimally Invasive Endovenous Therapies
Minimally invasive endovenous therapies include endovenous laser therapy. During this procedure, the surgeon makes a small incision in your skin and inserts an endoscope (a thin, flexible tube) into the affected vein. Endovenous thermal ablation users laser energy to cauterize (burn) and close abnormal veins that lead to varicose veins.
Open Surgery
Vascular surgeons perform two different types of open surgery for venous insufficiency:
- Vein ligation & stripping — This procedure involves maaking an incision, tying off the vein (ligation), and removing a long segment of the diseased vein.
- Microphlebectomy — This procedure incolves removing smaller varicose veins through a series of tiny skin punctures.
Preparing for Surgery or Endovenous Therapy
To decide which option is best for you, the vascular surgeon will perform an ultrasound exam. The goal is to look at the anatomy of the affected veins. If your veins are straight, you will probably be able to have minimally invasive endovenous therapy.
If your veins are curvy or twisted, the surgeon will likely recommend open surgery. Whichever option is best for you, the care team will let you know what to expect and how to prepare.
- Minimally invasive endovenous therapy is a same-day procedure using light sedation. It can take place at Area E of U of U Hospital or Farmington Health Center.
- Open surgery requires general anesthesia and is a same-day surgery that takes place at Area E of U of U Hospital or Farmington Health Center.
A week or two after your therapy, you will have a follow-up appointment with your vascular surgeon to see how the healing process is going and if your symptoms have improved. Even if the endovenous therapy or open surgery was a success, you may need to continue wearing compression stockings or continue managing your symptoms in another way, such as by exercising regularly.
Prognosis for Patients with Venous Insufficiency
Surgery may provide immediate relief if the only veins causing your symptoms are the superficial veins (those closest to the surface of your skin). However, a large percentage of people with venous insufficiency also have deep vein thrombosis (DVT).
DVT is a condition that happens when a blood clot forms in a vein located deep inside your body. These clots often form in the thigh or lower leg and can make symptoms of venous insufficiency worse. Treatment can include blood thinner medication, clot-busting medication, and endovenous therapy.
Make an Appointment
Referrals are required to make an appointment with a vascular surgeon at University of Utah Health. However, you do not need a referral for varicose vein treatment. To make an appointment, call 801-581-3495.
