Episode Transcript
Dr. Miller: You can't open your hand completely? Could you have Dupuytren's contracture? If you do, what do you do about it? We're going to talk about that next on Scope Radio.
Announcer: Access to our experts with in-depth information about the biggest health issues facing you today. The Specialists with Dr. Tom Miller is on The Scope.
Dr. Miller: Hi, I'm Dr. Tom Miller and I'm here with Nikolas Kazmers. He's an orthopedic surgeon here at the University of Utah in the Department of Orthopedics. Nick, what the heck is a Dupuytren's contracture?
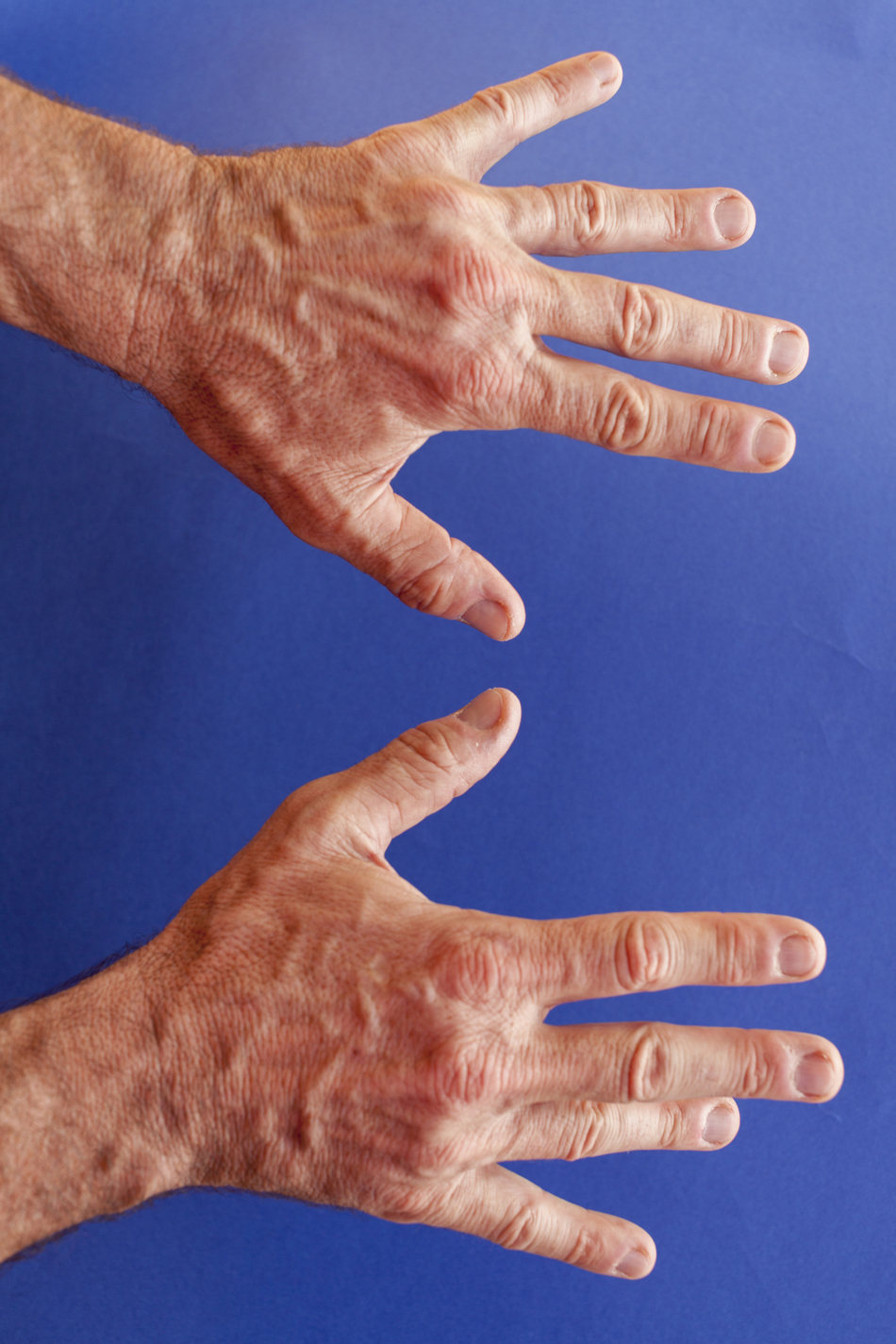
Dr. Kazmers: What it is is an abnormal thickening of some of the soft tissue in the palm of your hand or fingers and it can present either as a cord-like structure or a little knot or nodule, and then some patients even have bending of the fingers in which they can't straighten out the knuckle joints of the fingers.
Dr. Miller: So they can't open their hand completely? It's stiff and kind of rigid in this claw-like shape?
Dr. Kazmers: That's right.
Dr. Miller: Is that right, when it's bad?
Dr. Kazmers: That's right. When it's bad, that's what happens, and usually when it gets to that point, people seek help. I mean just tracing back in your average day things that you do, put the hands in the pockets to retrieve keys, grab your wallet out of your back pocket, or we have patients that are barbers or mechanics, they can't utilize their tools and work as effectively when the knuckles are bent down towards the palm side.
Dr. Miller: Does it affect certain fingers in the hand? Or is it all fingers? Or is it just one or two fingers?
Dr. Kazmers: It tends to affect the small and ring and long fingers, but it also can affect the index finger or even the space between the thumb and the index finger, and the nodules can be present throughout the palm, so it can involve any of those digits.
Dr. Miller: So Nick, who gets this? Young folks, older folks, in-between, or are you born with it?
Dr. Kazmers: Usually it's 40s to 60s where it becomes obvious. That's usually when the disease process starts. It is a genetic disease so in which it could be . . .
Dr. Miller: So the mom or dad might have had it or could a brother have had it?
Dr. Kazmers: Mom or dad may have it, grandparents may have it, siblings or blood relatives may have it, but it doesn't affect everybody in your family. It can skip a generation or sometimes your brother or sister may or may not have, and it definitely is a little more common in males than females as well.
Dr. Miller: Is it related to any other kind of other problem that one might have?
Dr. Kazmers: You can have similar soft tissue problems on the sole of your foot as well, nodules or cords on the foot. That's the most common other site.
Dr. Miller: What causes it? I mean you said it's genetic, but is there extra tissue around the tendon in the hand? What is it that causes this contracture?
Dr. Kazmers: So what this is, is it's normal tissue that undergoes an abnormal response in part because of one's genetic makeup. So normal structure in the hand called fascia, kind of the deep soft tissue under the skin, it contracts, has an abnormal amount of muscle cells in it, which can contract and that leads to the bending of the knuckles in which you can't straighten the fingers out, and it does lead to thickening of those structures too which you can feel in the palm of your hand or fingers as well.
Dr. Miller: Now, there are old treatments, and there's a new treatment and you're an expert in the new treatment. Tell me a little bit about the older treatments, and then let's go into the new treatment. And who do you reserve the new treatment for? Let's talk about that.
Dr. Kazmers: There are older treatments, which are still very effective and definitely have a role in treatment of patients today. Those typically involve surgery basically where there are incisions made in the palm or in the fingers where the cords or the nodules are and you remove a limited amount of these abnormal tissues and release the joints so that they can be straightened.
Dr. Miller: Does that work pretty well?
Dr. Kazmers: It works very well, and out of all of the available treatments that's known to have the lowest rate of recurrence, meaning the disease coming back, cords coming back, knuckles bending down in a stuck position.
Dr. Miller: So surgery which has been done for some time is very effective?
Dr. Kazmers: It is very effective. However, the downsides of that have to be considered, and those would typically be a little bit longer recovery period than the less invasive treatments.
Dr. Miller: How long?
Dr. Kazmers: Oftentimes it could be six weeks or so until you're doing gripping, barber going back to work, for example, probably about six weeks. No matter what we do it's usually night splinting with the fingers and knuckles straight for three to six months, so that's no different across the board, but it's really . . .
Dr. Miller: That's a long process.
Dr. Kazmers: . . . six or so weeks give or take, everybody is different until you're really gripping and doing a lot of manual labor with the surgical approach.
Dr. Miller: And what is new?
Dr. Kazmers: Sure, the newer treatment is actually a medication. It's an enzyme, meaning it's a type of medicine that can dissolve some of the abnormal tissue in these cords. It's interesting because it preferentially dissolves the cords, and it does not dissolve the other structures in the vicinity where you're doing the injection, and what that does is it weakens the cords. That's performed in the office. It takes about five minutes to do, and then the patient comes back anywhere between two and seven days after the medicine is injected and we manipulate the hand with some numbing medicine and it pops the cord and it allows the finger to go straight.
Dr. Miller: So basically the medicine kind of dissolves some of this fibrous tissue or makes it softer?
Dr. Kazmers: That's exactly right.
Dr. Miller: Interesting. What would be the downside of this? Is there a problem that it might affect the actual tendon or it could damage that?
Dr. Kazmers: The downsides basically include only a certain subsets of patients would qualify for such a treatment. You have to have a very, very distinct cord or rope in the palm of the hand so to speak, something that we can inject the medicine into and objectively pop that individual structure. Some people have more diffused disease, meaning it's not a distinct rope-like structure. It's spread out throughout the palm. That would not be a good situation for this newer medicine.
Tendon rupture, as you ask, has occurred. It's very, very low, and we believe the complication rate of this newer enzyme treatment, called collagenase or Xiaflex is the brand name, are lower than surgical treatment.
Dr. Miller: So how do you decide with a given patient whether you're going to start with an injection or advise surgery? Or can you do an injection first and if that doesn't work proceed to surgery? I mean what do you tell your typical patient who has rather severe Dupuytren's contracture? How do you make that decision with the patient?
Dr. Kazmers: Sure, you know, the general philosophy I have is to go through all the treatment options, go over expected rates of complication and rates of success and post-operative or post-procedure requirement as far as how much therapy or if therapy is involved, splinting or casting if that's involved, and help the patient make an informed decision. I think the days of paternalistic medicine are over, and I'd like to give the whole menu so to speak so they can choose the most appealing.
But when I do have a patient with Dupuytren's contracture, the first step is to make sure that, in fact, it is affecting their function. If there's a condition that's not affecting their function, it's harder to make them better in that regards. But I do like to counsel them to come back if the bending of the fingers are worse or if they do have dysfunction down the road, so I think that's number one.
Number two, it's important to understand what their dysfunction is, what their goals are, what they want to accomplish with a treatment, and that helps me guide them better.
Dr. Miller: So I'm thinking with the injection you're probably back to doing what you were doing before faster than with surgery. Is that part of the reason to do the injection?
Dr. Kazmers: Yeah, that's absolutely one of the appeals of the injection. The recovery is shorter than with surgery.
The third option, which we haven't talked about, is similar to the injection. It's non-surgical. It's done in the office. It's called a needle aponeurotomy, basically where the cord is numbed up with numbing medicine, and then a needle is used to poke little holes in the cord and then that is popped and the finger is straightened.
Dr. Miller: So it just loosens up that fibrous tissue. Basically just poke a needle in the area around the tendon.
Dr. Kazmers: Exactly.
Dr. Miller: How well does that work?
Dr. Kazmers: That works well. Additionally, again, that procedure is limited to people with a distinct rope or cord in the palm, similar to the collagenase treatment. But we can get a very quick correction in the office. It does not take very much time. The recovery is more along the lines of the collagenase, two to three weeks or so, depending on what the occupation and what type of activities the patient is trying to get back to, but certainly shorter than for surgical treatment.
The thought is that the recurrence rate is maybe somewhere between surgery, which is the lowest, and the collagenase is between that and the needle aponeurotomy, which probably has the highest rate of recurrence, maybe 50% in five years.
Dr. Miller: Then aponeurotomy has the highest rate of recurrence?
Dr. Kazmers: That's correct. And, again, low morbidity. It's quick and it's not expensive, unlike the collagenase, which is one of the drawbacks, different insurers vary on their amount of coverage of this newer medication.
Dr. Miller: It's expensive?
Dr. Kazmers: Yes.
Dr. Miller: So what's the recurrence rate there?
Dr. Kazmers: We haven't had really long-term data with huge numbers of patients, but we believe for surgery five years it's about 30%. Again, needle aponeurotomy five years probably about 50%.
Dr. Miller: And surgery . . .
Dr. Kazmers: And then the collagenase probably somewhere in the middle depending on the duration of the study. A lot of them don't have five years yet.
Dr. Miller: So poke, dissolve, or operate? Those seem to be the choices.
Dr. Kazmers: Poke, dissolve, or operate. Those are the choices.
Dr. Miller: You've nicely outlined the procedures that are available. How would you advise a patient who might have Dupuytren's to come and see you?
Dr. Kazmers: First and foremost, if they have concerns over what the diagnosis is, we're able to see them and we would be happy to see any patient where this is in question. We can confirm or refute the diagnosis just so they know what to expect. For other patients, they often have family members with this, so they're very well familiar with what their condition is and it is, in fact, Dupuytren's. For those patients who don't have any sort of functional limitations, what I would suggest is following this along with what we call a tabletop test.
What this is, it can be YouTubed or Googled if you'd like, but just to simply describe it, you have the palm of your hand down, you set it down on the tabletop and if you notice the knuckle joints off of the table, meaning you cannot get the knuckle joints flat onto the table, that would be indicative of some contracture of the fingers which we can worry about. I would encourage any patient with a tabletop test where they can't get the palm or the knuckles down to come in to be evaluated.
Announcer: Want The Scope delivered straight to your inbox? Enter your email address at thescoperadio.com and click "Sign me up" for updates of our latest episodes. The Scope Radio is a production of University of Utah Health Sciences.