Episode Transcript
Dr. Miller: EMG. It's easier than you think. We're going to talk about that next on Scope Radio.
Announcer: Access to our experts with in-depth information about the biggest health issues facing you today. "The Specialists," with Dr. Tom Miller, is on The Scope.
Dr. Miller: I'm Dr. Tom Miller and I'm here with Dr. Daniel Cushman. He's a sports medicine physician who uses electromyelography, or EMG. And, Dan, it's easier than people might think it is. I think there's some news out there from the past experiences of folks who say that it's painful. You hear about this on blogs and websites that you read. And I think that some patients come in and they're very nervous about having this procedure because they think it's pretty onerous, from what they've read. Talk about that. It's a lot different now.
Dr. Cushman: Definitely. I think this is one thing that I do where every day, when someone comes in, I have to talk them down before we even get started.
Dr. Miller: Really? Because they've looked it up online?
Dr. Cushman: They hear from their friends is the most common thing. Their friend will say, "Oh, I had this done to me. It was the worst thing ever."
Dr. Miller: And they're usually talking about an experience that was some time ago?
Dr. Cushman: Correct. Exactly.
Dr. Miller: So what is EMG? Let's talk about that first and then go into how you do it and why it's less painful or stressful?
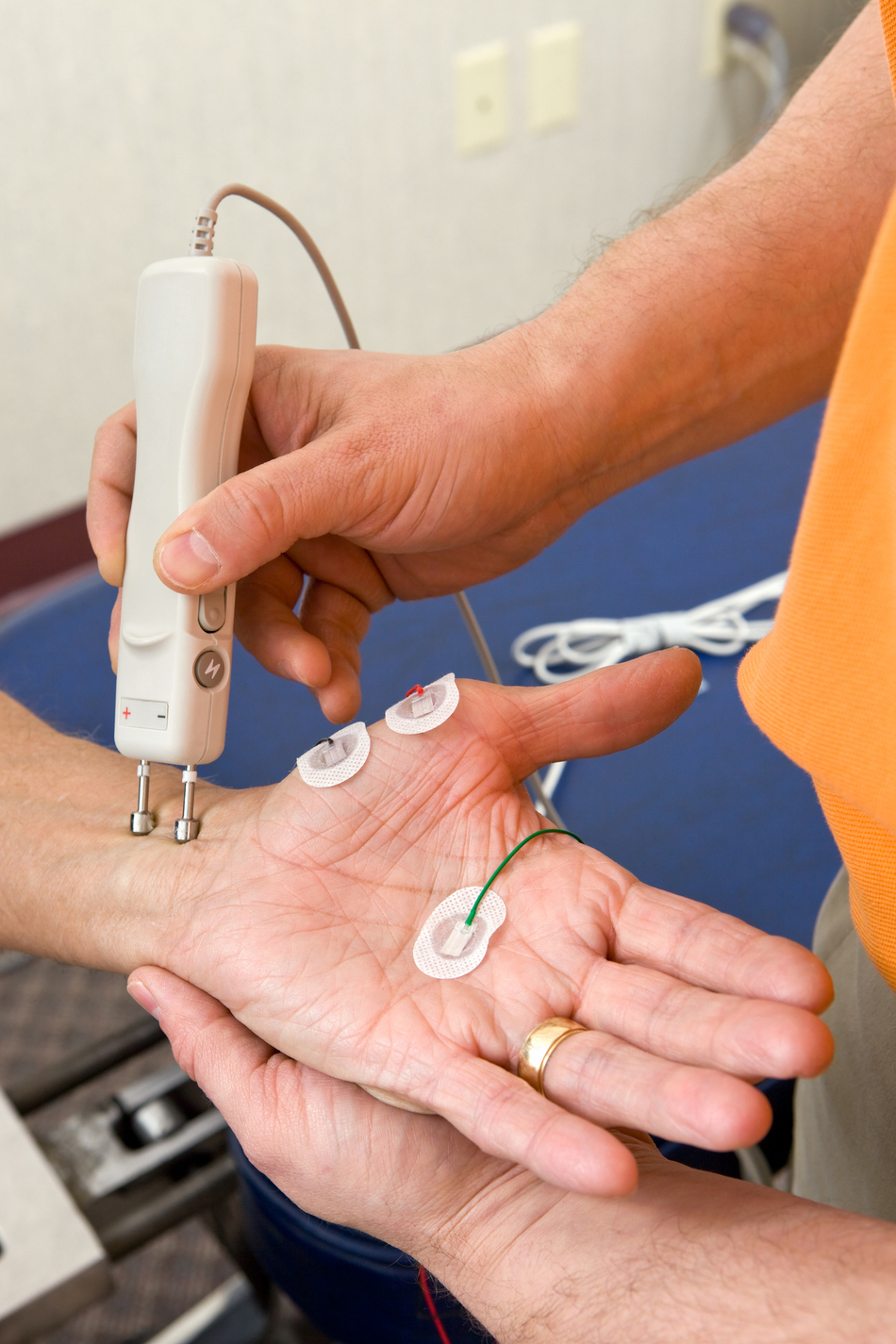
Dr. Cushman: So EMG talks about electromyography, which is looking at the electrical signals from the muscle. And the point of that is really to examine how well the muscles are working, how well the nerves are working, that go to those muscles. And there are two parts to the test. One is called the nerve conduction study. And what happens there is a small probe is placed on the nerve, on the surface of the skin, and a small shock is sent down the nerve. Just like in a wire, we can see how well that nerve is working by sending a signal down it. That's the first part.
Dr. Miller: Now, that sounds . . . you know, when somebody hears they're going to get shocked, they obviously think, "Uh-oh, this might be incredibly uncomfortable."
Dr. Cushman: Exactly. And so the way it works is that we just basically go up slowly on the electricity until they start even feeling it. They don't even feel it at the beginning. And then after they get . . . usually, the first one is the worst one. Then after that, they get used to it. It's kind of like when you rub your feet on carpeting, you touch something metal, nobody likes that sensation. But if you were to do that to yourself four times, by the fourth time, you'd be like, "Oh, I'm used to this."
Dr. Miller: It's like a little static shock.
Dr. Cushman: That's exactly it. Yeah.
Dr. Miller: So it's not like touching something coming out of a wall socket.
Dr. Cushman: Not at all.
Dr. Miller: Not at all.
Dr. Cushman: No.
Dr. Miller: Okay. Now, what about the needles? You use needles occasionally . . .
Dr. Cushman: Exactly.
Dr. Miller: . . . when you're doing EMGs.
Dr. Cushman: So the second part of the test is the actual EMG portion. And that's using a small needle about the size of an acupuncture needle, so really thin. And all we do is, we don't use any electricity, we just put it into different muscles along, in the body, depending on the test. So when we put that needle into the muscle, we can hear how the nerves are talking to the muscle. This part, on average, the pain level for people is somewhere in the range 3 out of 10. That's the most people will say it is. It doesn't really hurt. It feels more like a crampy sensation.
And when we do this, this gives us a lot of information. It can help us find if there's a pinched nerve, even though we're not really doing anything with the nerves. We're only doing the muscles. It can tell us a lot of information. It can tell us how old the problem is, if there's a new problem, if there's damage to the nerve, or if there's not damage to the nerve, and if things are getting better or have not started healing yet.
Dr. Miller: Talk about some of the common conditions where you use EMG to back up your clinical diagnosis.
Dr. Cushman: The most common that I do is probably carpal tunnel syndrome in the wrist. That's probably the most common. And then I would say the second most common would be a pinched nerve either in the neck or in the back.
Dr. Miller: So, basically, if you have . . . I mean, most of your patients are probably referred. Is that right?
Dr. Cushman: Yeah, most are.
Dr. Miller: And so you're getting patients from their referring providers who think they might have the right diagnosis, but they come to you to back up that diagnosis.
Dr. Cushman: That's correct. A good example would be a hand surgeon who . . . somebody might come in and say, "My fingers hurt," or, "My wrist hurts," or, "My hand hurts." And the surgeon can't particularly tell if that's coming from a pinched nerve in the neck or a pinched nerve in the wrist. And so, this test would help differentiate those.
Dr. Miller: So, obviously, not all patients need an EMG, but perhaps just a percentage of patients where the diagnosis is unclear.
Dr. Cushman: Correct.
Announcer: TheScopeRadio.com is University of Utah Health Sciences radio. If you like what you heard, be sure to get our latest content by following us on Facebook. Just click on the Facebook icon at TheScopeRadio.com.