Episode Transcript
Dr. Miller: Diagnostic ultrasound. We're going to talk about that next on Scope radio.
Announcer: Access to our experts with in-depth information about the biggest health issues facing you today. The Specialists with Dr. Tom Miller is on The Scope.
Dr. Miller: I'm Dr. Tom Miller and I'm here with Dr. Daniel Cushman. He's a sports medicine physician in the Department of Orthopedics at the Orthopedic Center here at the University of Utah. Daniel, welcome. Tell me a little bit about ultrasound-guided diagnosis of musculoskeletal disorders. I know this is a new technique, relatively new. It's been around for a long time but it's finding more applications these days.
Dr. Cushman: Definitely. Ultrasound is kind of a non-invasive way of looking at structures underneath the skin. It doesn't do a great job for things like bones which we have X-rays for, but if you're talking about something above the bone like a tendon or a muscle or those kinds of things, we can see those very well with ultrasound.
Dr. Miller: Does it assist you in your clinical diagnosis?
Dr. Cushman: All the time. For example, somebody hurts their shoulder, we can get a good look at those tendons, the rotator cuff tendons with ultrasound or if somebody's wrist is hurting we can look at the tendons there. Sometimes we can look at nerves particularly to see if they're being pinched somewhere.
Dr. Miller: It would help you, let's say, looking at a shoulder with an ultrasound, that might help you determine whether there was a full thickness tear or partial tear or even no tear.
Dr. Cushman: Exactly, and that's something that on exam when we're examining patients it's not something that's as obvious as it seems it should be. A lot of the time we can have patients who have completely torn their rotator cuff and they don't really have too many problems and then the opposite is true where somebody has done almost no damage to rotator cuff but they're in severe pain.
Dr. Miller: This would also help you decide on the guidance of treatment, right? Whether they go to physical therapy or whether you rest the shoulder for time.
Dr. Cushman: Exactly.
Dr. Miller: It just gives you a better sense of your diagnosis I suppose.
Dr. Cushman: All the time.
Dr. Miller: The other thing that's interesting is you're doing this right at the clinic visit, so this sort of obviates the need for having an MRI.
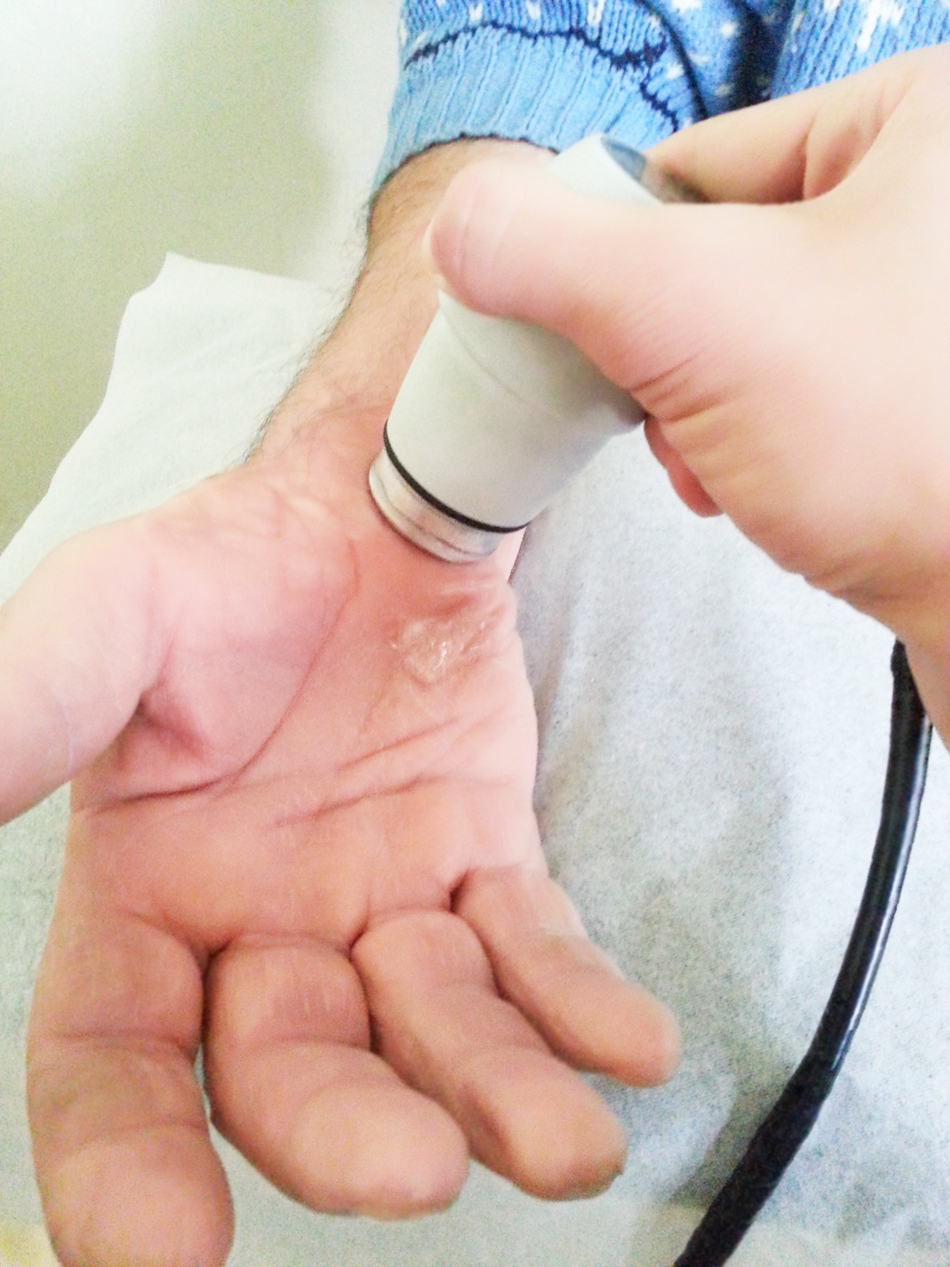
Dr. Cushman: Yeah. Definitely. A lot of the time I'll just simply grab the ultrasound machine with my patient in the room and it just takes a little bit of gel and that's pretty much it.
Dr. Miller: So this also maybe has a lower cost than the standard sort of other imaging techniques that we have.
Dr. Cushman: It's significantly lower and I don't know the exact numbers but probably somewhere in the range of a tenth the price of an MRI if you're looking at a shoulder for example.
Dr. Miller: Is it as good as good as an MRI for looking at, let's say again, a shoulder?
Dr. Cushman: Yes. That's really dependent more on the person doing the exam. If somebody has had a lot of experience with ultrasound, studies show they're about as good as an MRI. If somebody is not as experienced, then it's really only as good as the person who's doing the exam.
Dr. Miller: What other areas of the musculoskeletal system do you use this on? How about Achilles tendons or . . .?
Dr. Cushman: A lot of the time we can tell without having to use the ultrasound machine what the problem is but other times it's very helpful and so Achilles tendons, we do use it on occasion. There are there are some times where we think we know the diagnosis and this really either confirms it or shows us that something else is causing the problem and so it's helpful in that regard.
Dr. Miller: How about in the hip?
Dr. Cushman: In the hip joint there's a couple of uses for that pretty commonly. People who have had hip replacements where they can't really do an MRI afterwards and they still have some pain, a lot of times some of the hip replacement surgeons will have us take a look at the tendons that are going over the the prosthesis.
Dr. Miller: Sometimes patients will come in with pain and you've told me previously that you can use the ultrasound to sort of find out where that pain arises from or is there a structure along the nerve that is actually causing the pain. So for instance you might think it's . . . the patient may tell you that they have pain at the wrist or the end of the arm but actually the generation of that pain is higher up and you've learned that from the ultrasound.
Dr. Cushman: Yes, exactly. One of the one of the disadvantages of something like an MRI is you can really only do one segment at a time so you can only look at the neck or you can only look at the shoulder. You can't really do both at the same time. With an ultrasound, if you're thinking maybe a nerve is causing this, you can trace it all the way from the finger, all the way up the arm to the shoulder, to the neck and get a pretty full view of the entire nerve or whatever structure you're really looking for.
Dr. Miller: How many specialists like yourself are versed in using ultrasound as a diagnostic tool nowadays?
Dr. Cushman: Here at the U, there's probably about four or five of us at least in our department and it's getting more and more popular because it's such an easy test for patients. Patients generally love it by comparison to having to do an MRI or going back and additionally it's so much cheaper for the patient.
Dr. Miller: It also gives you real time feedback so that you don't have to wait for test results coming back from radiology.
Dr. Cushman: Definitely. A lot of the time, one other thing I was going to mention was that when patients say, "It hurts when I do this," and they move their arm or they move their leg, we can actually look at it while it's moving as opposed to an MRI or an X-ray, which only shows a static picture.
Dr. Miller: Do you think in the future that more orthopedic surgeons and sports specialists will be trained in this technique so that it's pretty common throughout the specialty?
Dr. Cushman: I think so. I think it's becoming kind of a second set of eyes for people to look under the skin.
Announcer: Thescoperadio.com is University of Utah Health Sciences radio. If you like what you heard, be sure to get our latest content by following us on Facebook. Just click on the Facebook icon at Thescoperadio.com.