What Is Dermatomyositis?
Dermatomyositis is an idiopathic inflammatory myopathy — an autoimmune disease of the skin and muscle tissue. In some patients the lungs may also be affected, and in others, dermatomyositis may be a sign of an underlying cancer. Other names for this disease include:
- amyopathic dermatomyositis (ADM) — this type has dermatomyositis skin symptoms without the muscle weakness,
- adult dermatomyositis, and
- juvenile dermatomyositis (JDMS).
Who Is Affected By Dermatomyositis?
This disease can happen to anyone at any age. However, adults in their late 40s to early 60s and children between the ages of 5 and 15 are more likely to be diagnosed with dermatomyositis.
Dermatomyositis Causes
The cause of this disorder has yet to be determined, but it is believed to be caused by an autoimmune reaction (when your body’s immune system mistakes its own healthy cells as foreign or unhealthy). Your genetic makeup may make you susceptible to developing the disease.
Find an Autoimmune Skin Disease Specialist
Dermatomyositis Symptoms
The first signs of dermatomyositis can make a sudden or gradual appearance over time. The telltale signs of dermatomyositis include:
- violet rashes that appear on your face, sun-exposed skin, and joints, such as knuckles, elbows, and knees,
- itchy, scaly rashes,
- sun sensitivity, and
- muscle weakness.
Adults may experience other symptoms such as:
- weight loss,
- low-grade fever,
- fatigue,
- shortness of breath, and
- calcinosis (calcium deposits that form under the skin or in the muscle). However, this symptom is more often seen in children.
This is a modal window.
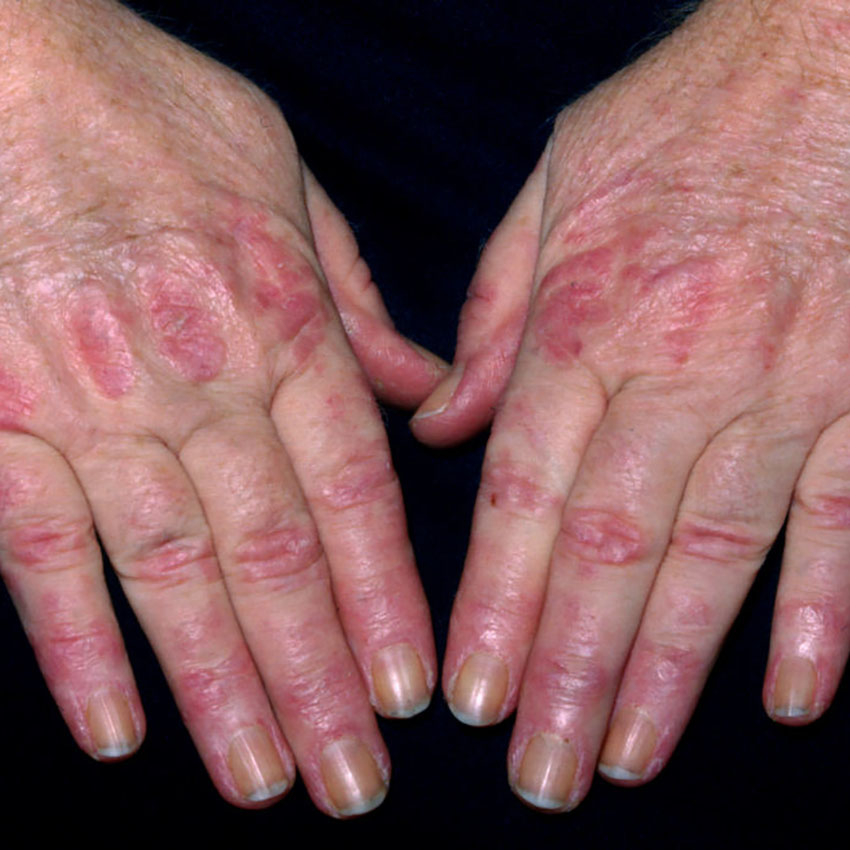

Dermatomyositis Rash vs. Lupus Rash
Dermatomyositis and autoimmune diseases like lupus may have overlapping features; however, the rashes look very different. A dermatomyositis rash has a purple-red hue that usually appears on your eyelids and joints like the knuckles, elbows, knees, and toes.
You may also find red rashes on your face, neck, shoulders, upper chest, back, and other places. A facial lupus rash typically resembles the shape of a butterfly that crosses the cheeks and bridge of your nose and looks like a sunburn. Other kinds of lupus rashes may look like red, scaly lesions that worsen after exposure to the sun.
Dermatomyositis Treatment
There is no cure for dermatomyositis, but there are treatments people should consider to help ease their symptoms.
- Topical medication — Corticosteroid creams may be prescribed to help with the rash and itch.
- Oral medication — A corticosteroid or immunosuppressant drug will often be prescribed to reduce inflammation.
- Sun protection — Wearing a hat, protective clothing, and using sunscreen with a high SPF when spending time outdoors is very important.
- Blood infusion — Biologic medications may be used to reduce inflammation. Some infusions are given on a monthly basis, whereas other medications may be given once or twice yearly.
- Physical therapy — This may be recommended to help maintain and regain your strength and range of motion.
We may even regularly screen you for cancer and lung inflammation using blood tests, CT scans, and other imaging tests.
Dermatomyositis Life Expectancy
If you treat it early, the prognosis for dermatomyositis is good. Some people may even recover and have their symptoms fully disappear, but this is more common in children. Patients who delay treatment may experience lung or heart problems or a permanent disability. It is important to monitor your symptoms closely and follow any instructions given by your physician throughout treatment to improve your overall health and outcome.
Make An Appointment with Our Specialists
A referral is required to meet with an autoimmune skin disease specialist. However, if you have questions about a skin condition without a pre-existing diagnosis, you can schedule an appointment with a general dermatologist at the U of U Health clinic by contacting 801-581-2955.
For new patients with an existing diagnosis, you will need a referral from your current provider. Your referral should include your name, date of birth, home address, phone number, and insurance company.
Before your first appointment, records about your autoimmune history should be faxed to U of U Health at 801-581-4911. These records should include clinic notes, biopsy reports, lab reports, diagnostic studies, radiographic studies, and treatments.
Please make sure your doctor faxes your referral to:
University of Utah
Department of Dermatology
Attn: Autoimmune Clinic
Phone: 801-581-2955, ask for autoimmune scheduling
Fax: 801-581-4911
We will review referral requests within 48 hours to make sure that the best dermatologist evaluates each case. We will contact new patients about an appointment.
