Episode Transcript
Interviewer: Lyme disease. What is it, what are the symptoms, and what you can do about it? That's next on The Scope.
Announcer: Health tips, medical news, research and more for a happier, healthier life. From University of Utah Health Sciences, this is The Scope.
Interviewer: Dr. John Kriesel is a physician and researcher in the Division of Infectious Diseases at University of Utah Health. And today, we hope to learn more about Lyme disease. Let's just start with the beginning, what is Lyme disease?
Dr. Kriesel: Lyme disease refers to Lyme, Connecticut, which is a region in the country that had a long-standing mysterious disease. It was later found to be due to a bacterium called Borrelia burgdorferi. So Lyme disease refers to infection with Borrelia burgdorferi.
Interviewer: All right. So how do you get this infection?
Dr. Kriesel: Well, Lyme disease is generally tick-borne infection and it's found commonly in the northeastern part of the United States. Also in the Midwest and the southeast part of the U.S., occasionally in the western U.S. You get it from ticks, generally, that harbor the Borrelia organism and then transmit it to people.
Interviewer: All right. So at some point, if you have Lyme disease, a tick got on your skin and did what ticks do, put their head in and gave you the bacteria?
Dr. Kriesel: That's right.
Interviewer: Okay. And there are some places in the United States that have it. There are some places that don't. Not all ticks carry it, it's just certain varieties. Is that correct?
Dr. Kriesel: Right. It's these Ixodes ticks. They're small ticks. There aren't many of them in Utah and we don't have any endemic cases in Utah that we know of. We've looked, believe me.
Interviewer: Yeah.
Dr. Kriesel: But we do have Ixodes ticks. We just don't have any Ixodes ticks that carry the Borrelia organism as far as we know.
Interviewer: Yeah, as far as we found. Okay. Who's at risk for Lyme disease?
Dr. Kriesel: Well, I think people that live in endemic areas are relatively high risk. And of course, I think men are at higher risk than women possibly because they get more outdoor exposure, typically. People who work outside in their yards or in their occupations often become infected.
Interviewer: What are the symptoms of Lyme disease?
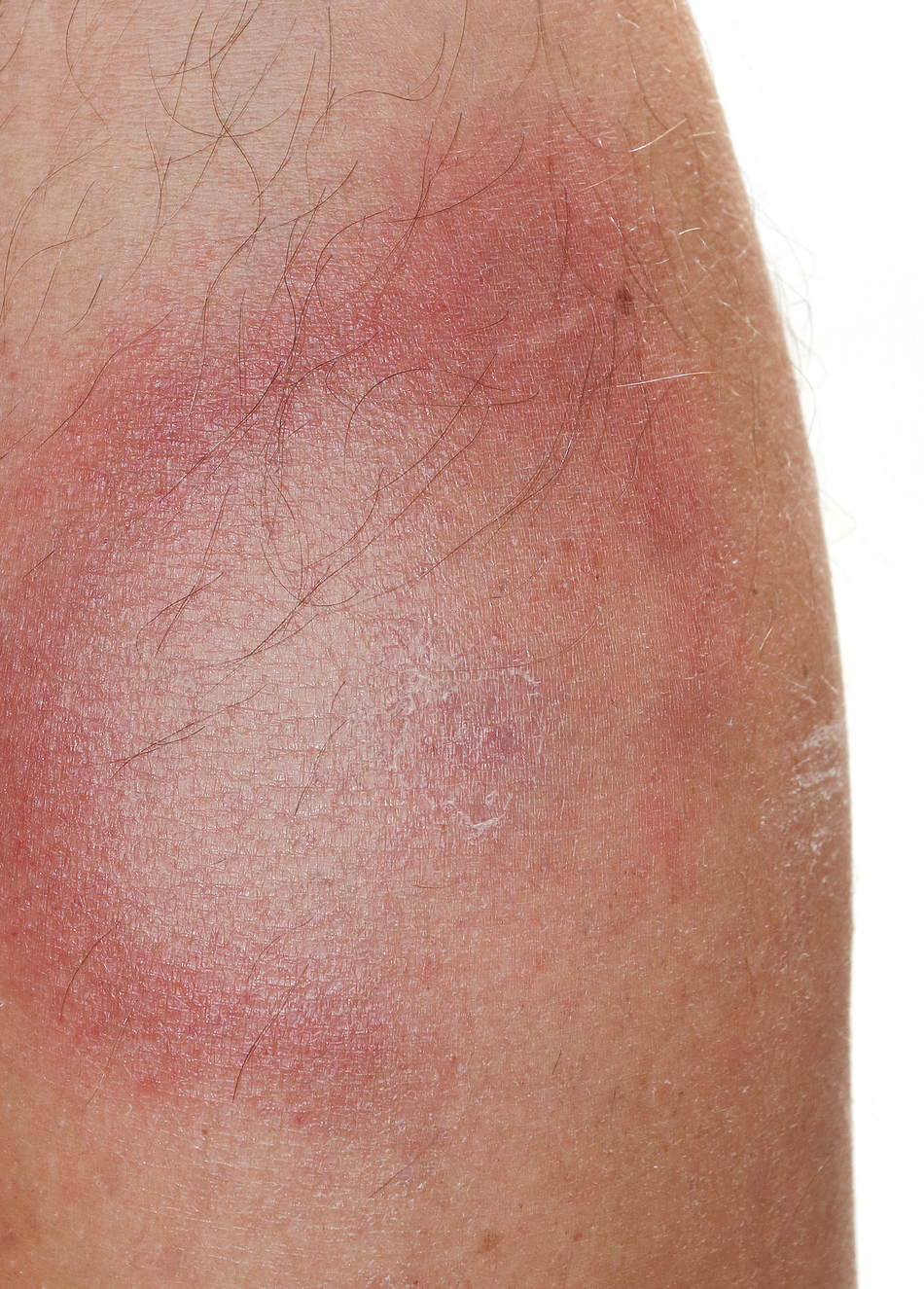
Dr. Kriesel: Well, people get an initial febrile illness and then they get a rash. I call it erythema migrans rash. You can certainly look up pictures of that, but that's considered to be . . . tick exposures, usually people don't find a tick because they're too small. But tick exposure in areas working outside or being outdoors and then getting an erythema migrans rash with a febrile illness.
Now, the illness often includes fatigue, lethargy, headache, sometimes neck stiffness, muscle aches, joint aches. And when patients travel in and they have a compatible illness, to Utah, we certainly ask them about possible tick exposure and then any rash that might develop.
Interviewer: And how do you diagnose that?
Dr. Kriesel: The acute disease is a clinical diagnosis, so you have to have exposure to an endemic area and then you have to have a compatible illness. Usually I think 80% are followed by the rash. So if you have those things, then you don't need to do a test. You just need to treat the patient.
Interviewer: Okay.
Dr. Kriesel: But chronic disease is harder. So somebody who has, say, a facial palsy, or heart rhythm abnormalities, carditis, or arthritis in one or more joints, or some sort of a neuralgia pain syndrome, this is a much more difficult thing to diagnose. And that requires antibody tests called serologic tests that we do in the blood.
Interviewer: So it really comes down to if you catch it early enough, if somebody sees a tick on them and then starts having these symptoms and gets the rash, pretty much case closed. You've got it figured out.
Dr. Kriesel: Right. Well, again . . .
Interviewer: As much as one could have a case closed in medicine.
Dr. Kriesel: Again, most people can't see the ticks because they're so small. But if they have a compatible exposure and a compatible illness, yes, that's a diagnosis of the acute illness.
Interviewer: But the trick is, somebody had an exposure, they didn't realize it. A few months later, they start experiencing some symptoms that they try to track down, then that's when you have to do the antibody test.
Dr. Kriesel: Exactly.
Interviewer: And it can be confused for a lot of other diseases, I've understood.
Dr. Kriesel: Well, it's a serologic test, so you're looking at antibodies that people make against Borrelia burgdorferi, right? Either by ELISA test or another test called the C6 Test or Western Blot Confirmatory Testing. So these are all special antibody tests, but there are other spirochetes in the world. So Borrelia are not the only spirochetes. Syphilis is a spirochete, Leptospirosis is a spirochete, so there could be cross-reactivity between diseases. So the first stage in serologic testing for Lyme disease involves an ELISA or an EIA, enzyme immunoassay test. And that's the screening test. It's like the HIV screening test, right, only it's for Borrelias.
And then if that's positive, then it goes on to a confirmatory test. The confirmatory test is called the Western Blot Test that involves specific bacterial antigens on a paper and then you see if there's antibodies that react to those antigens. So that's how that works and there are very specific criteria set forth by the CDC in these accredited laboratories to make that diagnosis.
Interviewer: And it could be a tricky diagnosis to make.
Dr. Kriesel: It could be tricky. It is tricky and frequently misinterpreted.
Interviewer: Lyme disease, probably prevented by keeping the ticks off you. Is that about the best way to prevent it?
Dr. Kriesel: Right. You can refer to the CDC. They have some specific recommendations. Actually, there's nice little brochures and I think the Utah Department of Health may have something similar.
Interviewer: All right. And then, if it's been determined that I have Lyme disease, what are the treatment options at that point?
Dr. Kriesel: That's a good question. I think we treat patients with doxycycline initially. There's also been some interest in treating possible exposures, post-exposure prophylaxis, but we don't really have occasion to do that very much here because the prevalence is so low.
Interviewer: So is this a shot? Is this some oral pills?
Dr. Kriesel: No, no, no, it's a pill. It's antibiotic pills.
Interviewer: An antibiotic pill.
Dr. Kriesel: And there are a number of different pills that could be used.
Interviewer: Okay. And then, is it ever completely treated or will you kind of have the symptoms or have the disease? It can only be controlled?
Dr. Kriesel: My understanding is the disease typically is cured, that the antibiotic treatment is curative. But there are always concerns about so-called post-Lyme syndrome. What are the diagnostic criteria for that? How do you make that diagnosis in patients? And that's kind of a more of a gray area. But can there be persistent infection? Well, not as far as I know.
Interviewer: Okay.
Dr. Kriesel: Right. But people can be re-infected and people can have difficult, prolonged infections and people may have symptoms that go on even after the spirochetes are eradicated.
Interviewer: That would be related to the fact that they did have Lyme disease?
Dr. Kriesel: Potentially.
Announcer: Want The Scope delivered straight to your inbox? Enter your email address at thescoperadio.com and click "Sign Me Up" for updates of our latest episodes. The Scope Radio is a production of University of Utah Health Sciences.