What to Expect After Hip Replacement Surgery
The following guidelines will discuss precautions to protect your new hip, exercises to increase your strength and range of motion, and techniques to manage activities of daily living to help you become an active partner in your care and recovery.
Normal Hip Joint
Your new hip is a ball and socket joint where the thigh bone (femur) meets the pelvis. A healthy hip has layers of smooth cartilage that covers the ball-shaped end of the femur and socket-part of the pelvis. The cartilage acts as a cushion and allows the ball of the femur to glide easily within the socket of the pelvis. The muscles around the joint support your weight and help move the joint smoothly so that you can walk without pain.
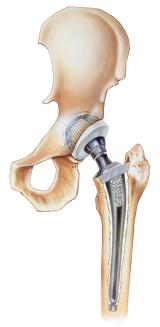
Your Replacement Hip Prosthesis
Your new hip prosthesis has a femur and pelvis part made from metal and plastics. The cup replaces the worn hip socket of your pelvis. The ball replaces the worn end of your femur. The ball is attached to stem that fits into your femur.
The cup and stem are sometimes cemented, or metals may have may have a porous surface that bone will grow into and create a tight fit. Your doctor and therapist will talk to you about positions to avoid after surgery. The best rule to follow is if a position or movement hurts, avoid it. If you suspect you have dislocated your hip, do not walk on it (call your surgeon and/or go to the emergency department).
Guidelines for Your New Hip Joint
Safety Tips for Home
- Use handrails on steps. Use low-heeled or flat shoes.
- Avoid wet or waxed floors.
- Keep your floors free of items you could trip on.
- Throw rugs or small objects should be kept off the floor for your safety.
- Watch for pets or other animals that could get in your way.
- Avoid ice or snow.
Sleeping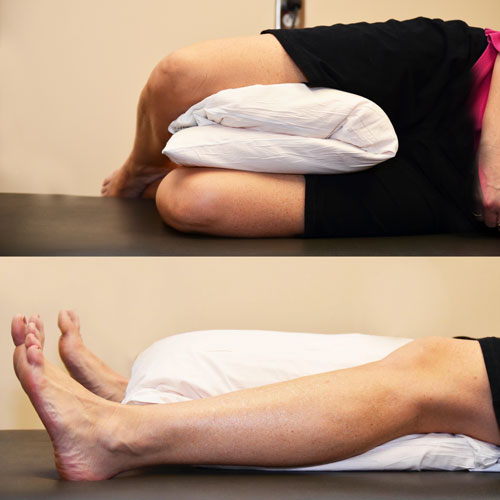
You will likely be most comfortable sleeping on your back with a pillow between your knees or on the opposite side of your new hip with a pillow between your knees. Sleeping on your stomach or on your new hip will be uncomfortable and should be avoided for several weeks after surgery.
Blood Clot Prevention
Follow your orthopaedic surgeon's instructions carefully to minimize the potential of blood clots, which can occur during the first several weeks of your recovery. Warning signs of possible blood clots in your leg:
- Increasing pain in your calf
- Tenderness or redness above or below your knee
- Increasing swelling in your calf, ankle, and foot
Warning signs that a blood clot has traveled to your lung:
- Sudden increase in shortness of breath
- Sudden onset of chest pain
- Localized chest pain with coughing
Notify your doctor immediately if you develop any of these signs.
Preventing Infection
The most common causes of infection following total hip replacement surgery are from bacteria that enter the bloodstream due to the following:
- Dental procedures
- Urinary tract infections
- Skin infections
Once you are past 12 weeks from surgery, you do not need to continue taking antibiotics unless you fall under the following high-risk categories:
- Uncontrolled diabetes (A1C >8, glucose > 200)
- Compromised immune system
- HIV/AIDS
- Rheumatoid arthritis or patients on oral steroids
- Active cancer
- Prior organ transplant or bone marrow transplant
- History of periprosthetic or deep prosthetic joint infection
Recovery for the First Three Months
How Long After Hip Replacement Can You Drive?
Most people can resume driving about 2–3 weeks after a hip replacement. You may resume driving under the following conditions:
- You are not taking narcotic pain medications.
- You don't have leg spasms.
- You have have full control of your leg.
You will need to continue taking extra precautions as you heal and recover.
How Long After Hip Replacement Can I Tie My Shoes?
It may take 6–8 weeks until you can tie your own shoes after a hip replacement. You may need to use slip-on shoes or adaptive equipment to take your shoes on and off during this period.
Can You Run After Hip Replacement?
How Long Does Pain Last After Hip Replacement?
You will have some hip pain for a few weeks after surgery. You will only need prescription pain medications for 5–14 days after the procedure. Most people can manage pain with over-the-counter pain relievers such as Tylenol (acetaminophen) after this period.