Announcer: Medical news and research from University of Utah physicians and specialists you can use for a happier and healthier life. You are listening to The Scope.
Interviewer: You found out your ultrasound that your child possibly might have a cleft lip. What should you do after that? What's going to be coming up and what are some things you need to know? Dr. Barbu Gociman is a plastic surgeon and a specialist in pediatric plastic surgery at the Cranial Facial Program at University of Utah. First of all, what is a cleft lip exactly? What's going on?
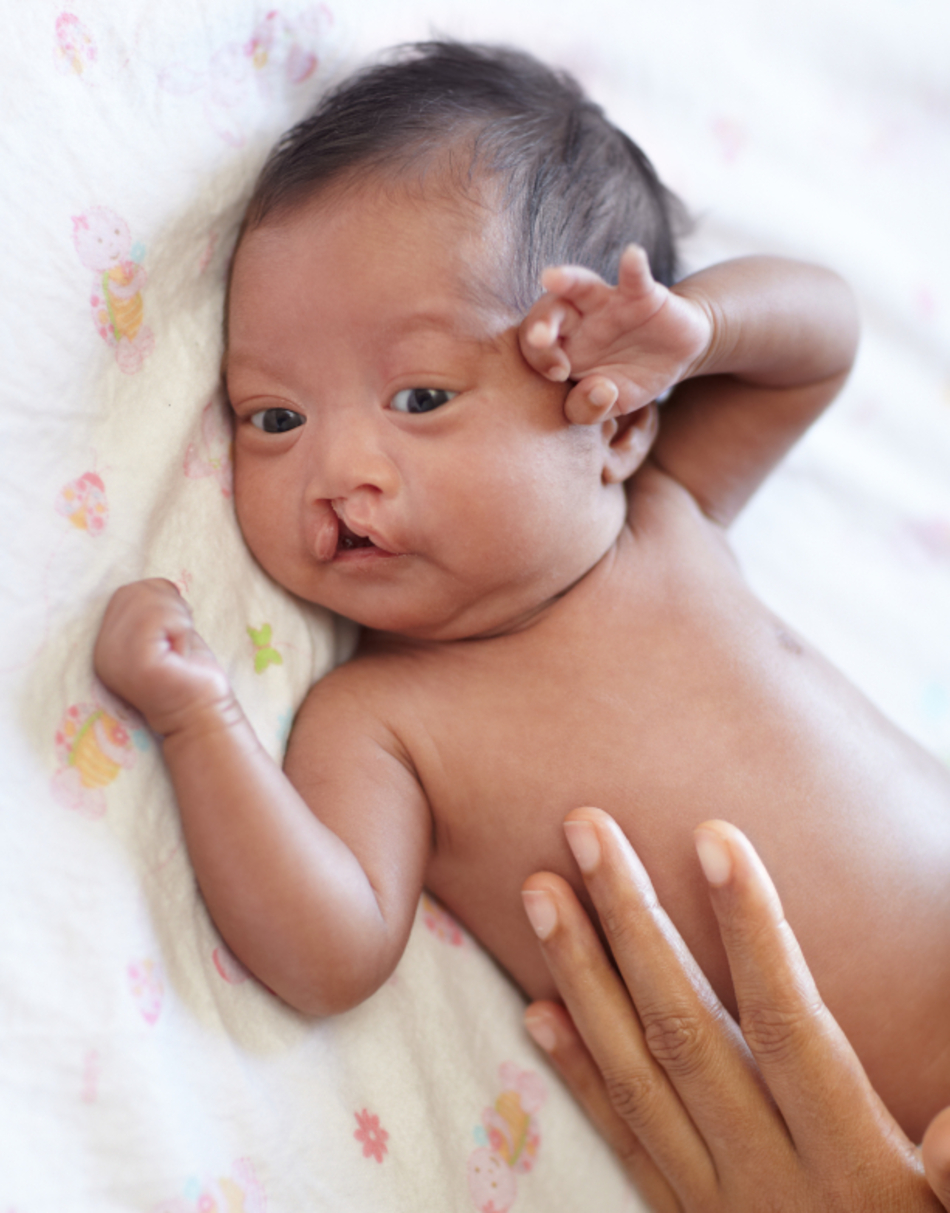
Dr. Gociman: Yes, it's not an extremely easy question to answer. It's anomalous and biologic developmental problem in which the forming face and particularly the lips, do not come together. It can be associated with a clefting of the palate. There are different degrees of clefting present. What a cleft means is basically an opening where, instead of the tissues coming together, they do not, and the bigger the defect, obviously the wider the gap between the elements that should come together.
Interviewer: So in the ultrasound meeting, they may indicate the there is a cleft lip possible. It could be very minor to very major. And what's that extreme?
Dr. Gociman: Yes, exactly. There is a whole spectrum. It can start with just a furrow that you can see on the lip which is not going to be present on the ultrasound. To mind comes, Joaquin Phoenix as an actor that has that deformity, as a personality that you can always look up. From that point you can have different degrees of deformities, just small degrees of notching in the lip. It can go all the way to the nose and extending to the alveolus, which is the bony part carrying the teeth, and all the way into back of the palate, which is the roof of the mouth, can be completely clefted.
Interviewer: And do the ultrasounds, do you have a pretty good indication of how bad it's going to be at that point? Or you could a parent be even surprised even more after the birth?
Dr. Gociman: Yeah, the ultrasound, obviously is a good modality to diagnose, but as any diagnostic modality, it's not 100%. So you'll not completely know the degree or exactly what structures are affected until you actually see the baby and you can examine him.
Interviewer: And that degree can mean the difference between maybe a single operation or many operations through the child's childhood, up until 18, 19 years old.
Dr. Gociman: Yeah, exactly. So there is a stepwise process that has been validated over the last 50 years or so, and obviously it continues to undergo refinements in how we treat these patients. So if only the lip is involved, usually one operation is enough to correct the deformity. The sequence of treatment for the more severe deformities involving the lip and the palate would be we start taping or do what we call a nasal alveolar molding, which would be reshaping of the structures and bringing them in a more anatomic position to facilitate the surgical repair. That is done by our orthodontist, Dr. Duane Yamashiro, and requires multiple adjustment. That will last for approximately for the first three months of life.
We usually do the lip repair around three months of life. At the same time we examine the palate, if the palate defect is really wide, we insert a palatal prosthesis, which is an obdurator that will facilitate feeding.
The second operation is done at around 10 months to one year of age, which is the soft palate repair. That is done right before the speech develops. We exchange usually the palatal prosthesis at the time if a large hard palate cleft is present. We repair the hard palate at around four years. At six years of age we do a repair of the clefted alveolus with bone grafting, if the baby has that problem. And finally we will do a formal rhinoplasty operation at the late teenage years if the nasal deformity is still persistent.
Interviewer: I would imagine one of the major concerns parents have is physical appearance. It sounds like there's also a lot of functional things that aren't going to be right if these surgeries don't happen. But as far as physical appearance, can you bring somebody back to the point where you couldn't tell they ever had a cleft lip?
Dr. Gociman: Unfortunately to completely, scarlessly repair somebody, it's not possible. We as humans we heal by scarring, so you'll always see a scar. The quality of the scar can be from a very, very thin line, which it's imperceptible to a person that is not very attune to what he's looking at, to a fairly thick scar that will require revisions or steroid injections or scar treatments. That is at the level of the lip.
As I said, because the nose is mis-shaped by the deformity, usually the eyes are going to be really drawn to that deformity. That's why we put a lot of effort in reconstructing the nose in a very anatomical fashion to try to avoid that from happening. We do the cleft lip repair at three months of age, just because we want the parents and everybody that comes in contact with the baby to see a normal baby. We do not want them to get used to the clefted baby.
All the other functional portions, the palate actually, functionally, the palate repair is much more important because the palate is involved in speech, is involved in swallowing. So functionally that is more important. But what we see, and it's human, we judge, where most of the people, the lip repair is the most important step and that is why we do it first, and that's why we pay a lot of attention to it.
Interviewer: I'm sitting here, hearing this and in a way my heart is breaking for parents that find out that this might be something that their child will have to face. How do you even address that? What do you say? How can people find comfort?
Dr. Gociman: It's definitely not an easy process. Fortunately, especially nowadays there are all the support groups. We can always put you in contact with the families that went through with our group. That brings a lot of comfort. It's very difficult, especially the first moment when you feel like you are all alone confronting with such a big, challenging problem. But our Cranial Facial Program at the University of Utah has the answers and we are very happy to address all of them multiple times. Our phone number that you can reach us is 801-581-7719. The Cranial Facial Center is the way to go.
Announcer: TheScopeRadio.com is University of Utah Health Sciences Radio. If you like what you heard, be sure to get our latest content by following us on Facebook. Just click on the Facebook icon at TheScopeRadio.com.